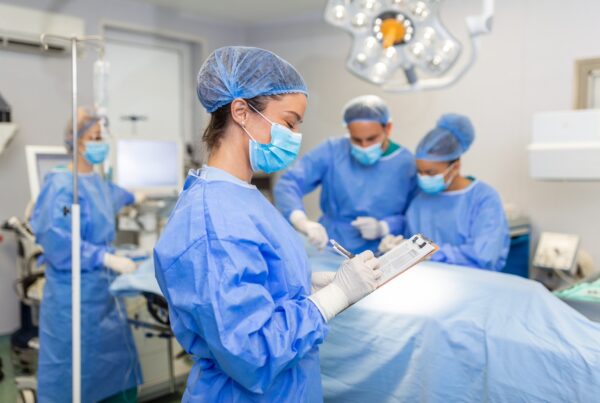
Patient safety is a critical component of patient care and Sterile Processing Department (SPD) plays a vital role in ensuring a safe patient outcome. It is paramount to patient safety in the operating room that clean and sterile instruments, which function properly, are readily available to the surgical team. Any breakdown in sterilization and processing of surgical instruments may lead to post-op infections, surgical errors and delays that could affect optimal patient outcomes. The SPD staff face many challenges in performing their roles, some of which stem from lack of education, compliance to policies, standards or procedures, and lack of performance criteria to monitor the quality of their work.
Staff Education and Certification
In today’s world it is becoming more and more common for facilities to hire staff members who have little or no previous experience and/or training in SPD. This may be due to lack of experienced candidates in the specific hiring area or may be due to a budgetary constraint. Contracted staff is often used as a temporary means until regular qualified staff can be secured. The primary challenge with hiring inexperienced staff is that time and resources needs to be invested before a facility can start to see a return on their investment. An additional challenge, which is just as daunting, many SPD departments lack a dedicated educator. The responsibility for the education and training of new hires, as well as tenured staff members, often falls on the shoulders of the most senior technician. The senior technician may not always possess the appropriate skillsets, training or experience required to be an effective educator. This additional responsibility creates conflicting priorities and further leads to SPD burn-out. It is critical that each SPD department have a dedicated educator to fully focus on the training of new hires and current staff to address SPD specific issues and opportunities.
Certification is mandatory in some states and is required is many hospitals currently. The subject of certification can be challenging for some individuals. Fear of testing, being overwhelmed by regulatory agency policies, rules and standards, and microbiology theory, that may be new and not well understood, can present challenges for these individuals.
Compliance to Policies, Standards and Procedures
According to ANSI/AAMI ST79, “the health care organization should establish policies and procedures for all methods of cleaning and decontamination of reusable items”. A policy or procedure written by a facility but not followed by the SPD staff puts patients and staff at risk. An instrument not processed in accordance with manufacturer’s instructions, Instructions for Use (IFU), cannot ensure its effective decontamination and proper sterilization and should not be considered safe for patient care. It is paramount that the IFU provided by the manufacturer always be followed.
Over my SPD career I cannot tell you how many times I have heard comments like, “I am not sure what the policy says but we have always done it that way,” or “I don’t have time to look up the IFU.” The sad truth is that in the hectic day to day scramble to process instruments and support patient care, we tend to become complacent in compliance with written directives. When the focus becomes fully on quantity over quality the risk of making a mistake, or just doing something wrong, dramatically increases, and thereby significantly raises the risk to patient safety. Compliance to written directives is not just important, it is imperative to a positive patient outcome and is the cornerstone to patient safety.
Quality initiatives in the SPD: Audits and Proactive Program
The direction in today’s healthcare environment is the focus on value-based healthcare, where quality and efficiency are the ultimate goal. No longer should we just be counting widgets, but we should be looking at quality over quantity of those widgets. This is not to say quantity is not important for resource planning and management, but as it relates to patient safety, we should focus on quality. How does that apply to SPD, which is so far removed from direct patient contact, you ask? First, we ensure a robust proactive quality audit program is in place which allows you to monitor for patterns in an objective manner. These quality audit programs are helpful in signaling potential problems and risks, before they come to fruition. Audits should include such items as inspecting instruments (functionality, cleanliness), inspecting containers and filters for defects, ensuring chemical integrators are in the set etc. These audits should be documented to help track how you were able to resolve the defects.
Summary
Essential to patient safety is a well-trained performing staff that is not only familiar with governing written directives, but also complies with them. We ensure that our staff lives up to those standards by implementing an active continuous education program and proactive quality audit programs which allow us to recognize potential issues and mistakes before they happen. Patient safety is SPD’s primary goal to ensure best outcomes.